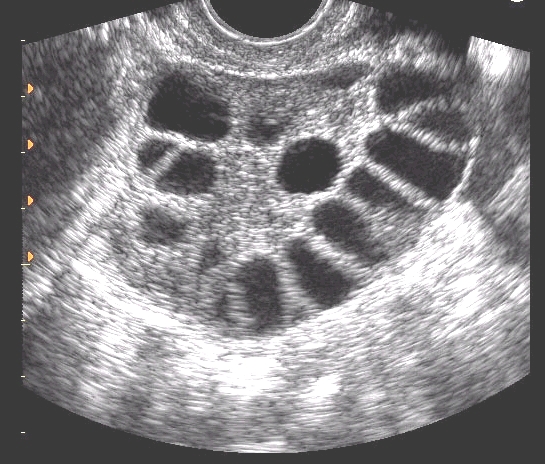
In Vitro Fertilisation
What you need to know about IVF/ICSI
The following information explains briefly the procedures of In Vitro Fertilisation (IVF) and Intracytoplasmic Sperm Injection (ICSI). This will give you an understanding of the treatments and an outline of methods we use here. We will be happy to discuss any questions you may have about the treatments.
What is IVF?
IVF is the technique of mixing the women's eggs with sperm from her partner in a small dish or test-tube in the laboratory to allow fertilisation to occur. Once the eggs are fertilized (at this stage known as embryo), one or more embryos are replaced into the woman's womb through the cervix.
Who needs IVF?
Originally IVF was performed only on women with tubal factor infertility. Now, IVF is performed for every type of infertility. For some types of infertility, IVF is usually done as a first line treatment, bypassing all more conservative treatments.
FIRST LINE TREATMENT
1. Severe male factor infertility– This includes men with an extremely poor semen analysis, including men with decreased sperm concentrations, motility or morphology parameters. This group also includes men with obstructive azoospermia, which describes a subset of men who make sperm, but some part of the duct system is blocked, as in men who have had a vasectomy. These men may require a surgical procedure, such as a testicular biopsy or epididymal aspirate to retrieve sperm. For couples with severe male factor infertility, a procedure called intracytoplasmic sperm injection, ICSI, is required. With ICSI, individual sperm are injected into individual eggs to promote fertilization.
2. Tubal factor infertility/pelvic adhesive disease– Women with damaged or absent tubes that are not surgical candidates for tubal reconstructive surgery or whose prognosis is very poor with surgery.
Often women attempt less aggressive forms of fertility treatment before doing IVF, such as artificial insemination in combination with clomiphene citrate or injectable gonadotropins. If they fail to conceive with these more conservative treatments, they are candidates for IVF.
OTHER INDICATIONS
3. Ovulatory dysfunction– The ovaries are not producing eggs in a normal manner or egg production is diminished with age. Women with polycystic ovarian disease fall into this category.
4. Endometriosis– The presence of endometrial tissue outside of the uterus and in the pelvis.
5. Uterine factors – Disorders of the uterus that lead to decreased fertility, such as fibroids.
6. Unexplained infertility– After a thorough workup, no cause of infertility can be found. These women are ovulatory, have normal tubes and ovaries, no endometriosis and their husbands have normal sperm.
7. Other causes– This includes people with chromosomal problems, immunological problems and serious illnesses.
What does IVF involve?
Below is a short outline of the steps involved in IVF. These include
- Pre-treatment evaluation
- Stimulation of the ovaries
- Monitoring of egg development
- Egg collection
- Sperm preparation
- Fertilisation
- Embryo transfer
- Pregnancy test and scan
Pre-treatment evaluation
|
NO |
TESTS/CHECK-UP |
WIFE |
HUSBAND |
|
1 |
Serology: Haemoglobin RBC PCV MCV MCH MCHC RDW Blood group |
√ |
√ |
|
2 |
RPR (VDRL) HIV 1&2 Ab/Ag Hepatitis B antigen Hepatitis B antibody Hepatitis C antigen Hepatitis C antibody These tests can be done in home country. |
√ |
√ |
|
3 |
Semen Analysis: Total count/ml Motile count/ml Progression % Normal morphology (shape) % Count after washing Please advise if husband needs PESA/TESA |
|
√ |
|
4 |
Baseline Reproductive Hormone (to be done once between Day 2-Day 6 of cycle): Follicle Stimulating Hormone (FSH) Estradiol (E2) Lutienizing Hormone (LH) Progesterone (P4) Thyroid Function Test Prolactin
|
√ |
|
|
5 |
Pelvic examination and ultrasound assessment report |
√ |
|
|
6 |
Menstrual cycle pattern |
√ .
|
|
|
7 |
Medical history: Drug allergy (if any) Previous surgery (if any) Illnesses (eg. Asthma, if any) |
√ |
√ |
Once all tests and data have been completed, patients can proceed to start their treatment i.e stimulation of the ovaries on Day 2 of their next period.
Stimulation of the ovaries
In a natural menstrual cycle, a woman produces only one egg, but in order to increase the chances of pregnancy in IVF it is desirable to stimulate the ovary to produce several eggs. This is done by giving you hormone injections for about 12 days to make the eggs grow. The eggs need to be exactly "ripe" at the time of their collection and so their development must be carefully monitored. The drug treatment varies slightly to suit your circumstances such as age and FSH level, but this will be fully discussed with you beforehand.
Monitoring of egg development
Development of the eggs is monitored by 2 methods. First the size and number of egg follicles growing in the ovary are observed by ultrasound scanning. The scan is obtained by passing a small transducer into the vagina and a clear picture of the ovaries can then be seen on a television screen.
The second method of monitoring is by measuring the hormones produced in the ovary This is done by a blood test. The blood test and scan will be done about 2-3 times during the 2 weeks before egg collection. At least three eggs must be growing before we can proceed to egg collection. Sometimes treatment will therefore fail at this stage. If the stimulation treatment has been successful, the eggs will be ripe at the right time and a final, different injection will be given to complete the ripening. Egg collection will be planned for about 36 hours after this injection. On rare occasions a complication of this treatment can occur (Hyperstimulation Syndrome). The ovaries may become large and painful and if severe, admission to hospital may be necessary. This usually only occurs if you become pregnant and gets better within a few weeks.
Egg collection
Eggs are collected from the ovary by suction through a fine needle. This needle is inserted into the ovary through the vagina using the ultrasound picture as a guide. You have a choice of full general anesthesia or sedation, depending on your current health status and medical history. We hope to obtain at least 3 eggs but usually larger numbers are obtained.
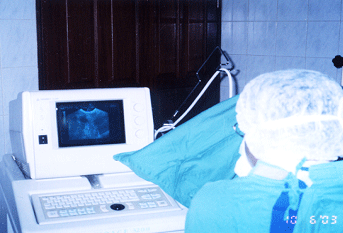
Trans-vaginal Ovum Pick-up Procedure in the theatre.
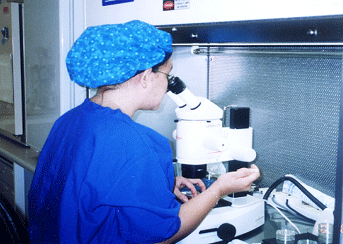
An embryologist will promptly check if an egg was collected.
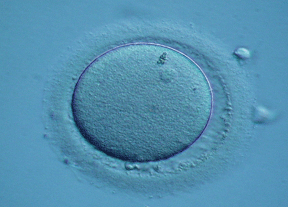
A mature egg.
Sperm preparation
We will inform you of the approximate sperm collection time once the ovum pick-up time has been arranged. It will be approximately 3 hours after the operation. Three days abstinence from intercourse will be necessary prior to ovum pick-up. Instruction will be given to couple prior to ovum pick up. The sperm sample is produced by masturbation at the Centre or by other means by arrangement. There is a room for this purpose. You are asked to wash your hands beforehand to minimise the chance of contamination. Lubricants are NOT to be used.
It can be very difficult for some to produce a sperm sample on request under these conditions. If you are worried about this aspect of the programme, please discuss it with us at or before the start of the treatment cycle, so that arrangements can be made to freeze some semen if necessary - freezing must be done at least a week before egg collection. Sexual activity may be continued as usual until three days before the time of the wife's egg collection. Abstaining from then on is important to allow the sperm to reach optimum quality.
A fresh sperm sample is needed for IVF so that the sperm are of good quality. The sperm are specially prepared so that only the best, cleaned sperm are put with the eggs.
Fertilisation
After collection the eggs will be put into the incubator for a short time. A relatively small number of sperm are then added to each egg. They will then be kept in the incubator for about 2 days. They are looked at daily and we will keep in touch with you by telephone and advise when to attend for embryo replacement.

Placing the eggs and sperm in the incubator.
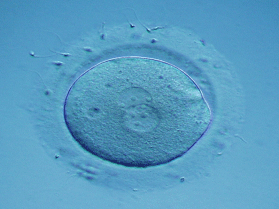
A fertilised egg
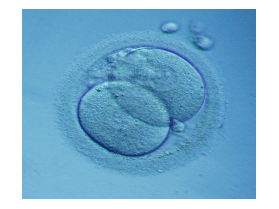
Embryo with two cells
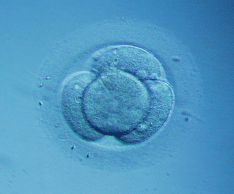
Embryo with four cells
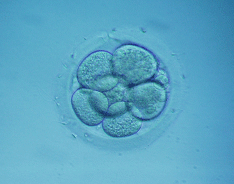
Embryos with eight cells
Intra-cytoplasmic Sperm Injection (ICSI)
For ICSI, fertilization is done by injecting a viable sperm to each egg. The mature egg is held with a specialized holding pipette. Then, a very delicate, sharp and hollowneedle is used to immobilize and pick up a single sperm which is injected in to the cytoplasm. The injected eggs are placed in an incubator and will be checked the next morning for fertilization.
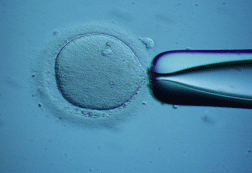
The mature egg held with a pipette.
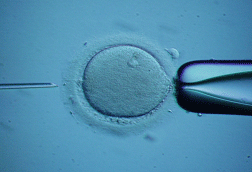
Then, a very delicate, sharp and hollowneedle is used to immobilize and pick up a single sperm.
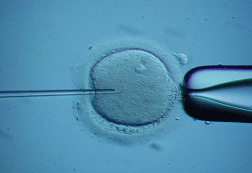
Sperm is injected into the cytoplasm.
Embryo transfer
An opportunity to discuss how many embryos should be replaced will already have taken place. The chances of pregnancy increases with the number of embryos replaced, but so does the risk of multiple pregnancy. There is an increased chance of losing one or all of the babies in a multiple pregnancy and we are therefore anxious to avoid this complication. We usually recommend no more than 3. The procedure for replacement of the embryos is virtually painless and is little more than an internal examination. You will not need to lie down afterwards and then you can return to normal (but not too strenuous) activity.
Sometimes there are more embryos available than we can replace. In this case, you may consider freezing and storing your surplus embryos for future use.
Pregnancy outcome
After IVF further injections or pessaries may be needed to support the lining of the womb. You can do a pregnancy test about 2 weeks after egg collection in your home country. If this is positive, a scan will be performed 5 weeks after egg collection to confirm that it is a good pregnancy and that a baby is growing. Miscarriages can occur in any pregnancy but there is also no increased or decreased risk after IVF. There is a small (7%) chance that the pregnancy may stick in the tube (ectopic pregnancy) If this occurs an operation is required to remove the pregnancy and possibly the tube as well. We see everyone who becomes pregnant regularly at the hospital until we are sure that the pregnancy is growing normally and we hope you would be able to see your doctor in your home country for further follow-up.
Disappointments
Clearly these methods of treatment are complicated and stressful and they may fail at any stage. Sometimes we can explain why it has failed but often it is for reasons which we don't understand. If you are not successful we will arrange for you to discuss what happened in detail via phone or email. If you have any further questions about these treatments, the medical and nursing staff at the centre are available to answer them.
You will be asked to attend for a further counselling/ information session at the Concept before treatment begins which will give you both an opportunity to discuss any problems.
Enquire from us
Send an enquiry to us now and get a Free Consultation for your visit.