Female Infertility
For a woman, creating a baby is complex; there are many stages and much is involved. With all this complexity, there are many possible causes of female infertility; it's a very complicated problem. In fact the issues involved with female infertility are far more complex than male infertility. Even with many possible causes, there are some that we see quite regularly, these include:
AGE
With the advancement of women socio-economically, many are delaying marriage and child-bearing. This has resulted in an increase of women seeking pregnancy in their mid-thirties and early forties. Although there is a very well demonstrated decline in female fertility as a function of age, this phenomenon has typically has been under-recognized not only by the general population, but also by many health care providers. This is probably related to the fact that in previous decades women generally had completed childbearing by the late 30’s and in fact many of the pregnancies that occurred in the later reproductive years were unplanned. An increased awareness of the effects of aging on fertility for patients and health care providers is critical to the prevention of age-related infertility. It will encourage patients to avoid delaying treatment once they reach the critical age group.
Compared to other major organ systems, the female reproductive system ages to the point of failure at a relatively young age. There is a gradual loss of fertility as a function of female age with the rate of decline in fertility becoming more dramatic after the age of 35. This decline in fertility occurs in spite of the fact that women generally maintain regular, ovulatory menstrual cycles well into the fifth decade. The impact of age on women’s fertility is demonstrated in:
a) The declining number of oocytes which are not renewable.
b) The increased number of abnormal oocytes resulting in abnormalities during metaphase stage of meiosis II.
c) The increased number of embryos that are likely to be implanted.
ANOVULATION
There are many causes of anovulation (the absence of ovulation) and a range of symptoms. Some of the causes are treatable with drugs and sometimes lifestyle changes. Others are not treatable and pregnancy may only be possible with the help of an egg donor.
Some treatable causes are:
- Hypothalmic anovulation - caused by exercise, stress and/or weight loss
- Hyperprolactinemia - raised levels of prolactin, a pituitary hormone
- Polycystic ovarian syndrome (PCOS).
Polycystic Ovary Syndrome
Polycystic ovary syndrome (PCOS) is the most common endocrine disorder in women, affecting an estimated five to ten million women of reproductive age. For women trying to conceive a child, PCOS is a serious, common cause of infertility - nearly half of all female factor infertility cases can be traced to PCOS. New medical insight into the disease has led to treatment options, including insulin-reducing ovulation medication (clomiphene, glucophage, Metformin), dietary changes (low glycemic diet) and surgery (ovarian drilling), which have proven successful and allow many women to overcome PCOS and conceive a child naturally, while reducing the risk of miscarriage. Women who undergo treatment for PCOS but are still unable to conceive naturally often turn to assisted reproductive technologies, including IVF, and experience high pregnancy success rates.
Polycystic ovarian syndrome is a common cause of anovulation and infertility in women. Women with this syndrome do not ovulate regularly and have ovaries that contain multiple small cystic structures, usually about 2-9 mm in diameter. This gives the ovaries a characteristic "polycystic" (many cysts) appearance on ultrasound.
Polycystic ovarian syndrome causes irregularities in the menstrual cycle, and sometimes a total lack of periods - amenorrhea
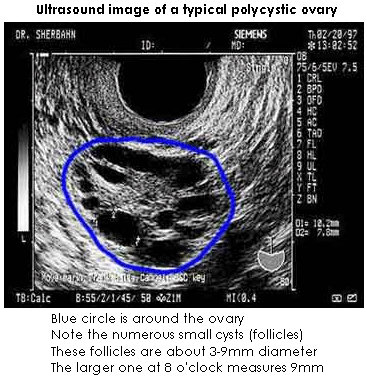

For comparison, an ovary with a mature follicle at midcycle in a woman that ovulates monthly.Blue circle is around the ovary, the black area is the fluid in the follicle. The follicle is mature size (here 20mm diameter) and contains a microscopic egg (not visible on ultrasound)
The basic problem is that although the polycystic ovaries contain many follicles with eggs, the follicles do not develop and mature properly so that they do not ovulate. Women without polycystic ovaries normally develop one mature follicle each month which ovulates (releases) one egg.
Women with polycystic ovaries are often hyperandrogenic as well. This means that their ovaries produce an excess amount of male hormones testosterone and androstenedione which can cause increased hair growth - hirsutism, and sometimes other problems as well, such as weight gain, diabetes, cardiovascular disease. The typical story seen in women with polycystic ovaries is irregular menstrual cycles, onset of hirsutism in the teens or early 20s, and gradually worsening excess hair growth.
When they attempt to get pregnant, women with polycystic ovaries will usually have difficulty. Some women with this disorder will ovulate (release a mature egg) occasionally, others do not ovulate at all. In order to conceive, sperm must be able to find and fertilize a mature egg. Therefore, they will usually need to undergo induction of ovulation to get pregnant.
The good news is that pregnancy rates are high for women with this condition. The large majority will be able to have a baby, if they will undergo treatment. Many will be able to get pregnant using fertility hormone pills to induce ovulation. This is often given by general gynecologists. About 75% of women with polycystic ovaries will ovulate with clomiphene, but only about 40% will get pregnant with it.
If this fails after about 6-9 ovulatory cycles, the next step is usually injectable gonadotropins. About 90% of women that do not ovulate with clomiphene will ovulate with this medication. The majority will get pregnant as well.
If this fails after about 3-6 ovulatory cycles, the next step is usually in vitro fertilization. The majority of women with polycystic ovaries that have not gotten pregnant with the above treatments will conceive with IVF.
BLOCKED FALLOPIAN TUBES
Tubes can be blocked for a number of reasons:
- Blocked from birth (congenital tubal obstruction)
- Intentional tying or clipping (to prevent pregnancy)
- Accidental damage following other surgery e.g. colectomy
- Severe endometriosis
- Inflammation (salpingitis).
Of these, the last is by far the most common.
Salpingitis
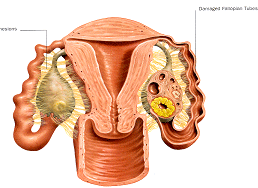 Inflammation of the fallopian tubes can occur from the inside, that is, from the uterus, as is the case with sexually transmitted diseases such as gonorrhoea or chlamydia. It can also come from outside the tube by the spread of infection from another organ such as the appendix. When this happens, the tube is often damaged by adhesions, where two damaged surfaces actually join together. Adhesions can also occur after pelvic surgery or as a result of endometriosis. Adhesions can obstruct in a number of ways - by separating the ovary and tube with new tissue or by blocking the outer end of the tube. In many cases, microsurgery can be helpful in clearing the blockage.
Inflammation of the fallopian tubes can occur from the inside, that is, from the uterus, as is the case with sexually transmitted diseases such as gonorrhoea or chlamydia. It can also come from outside the tube by the spread of infection from another organ such as the appendix. When this happens, the tube is often damaged by adhesions, where two damaged surfaces actually join together. Adhesions can also occur after pelvic surgery or as a result of endometriosis. Adhesions can obstruct in a number of ways - by separating the ovary and tube with new tissue or by blocking the outer end of the tube. In many cases, microsurgery can be helpful in clearing the blockage.
Hydrosalpinx and pyosalpinx
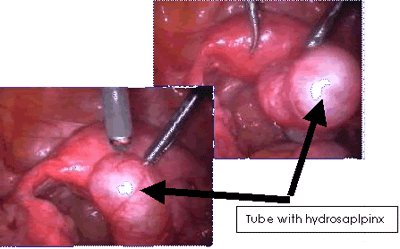
A hydrosalpinx is a particular type of tubal blockage in which the tube is obstructed near its fimbrial end. The tube becomes filled with clear watery fluid. Sometimes after IVF the rise in progesterone causes the tube to relax and this fluid can be passed into the uterus, washing out the transferred embryo. This process accounts for quite a few cases of persistent IVF failure.
A pyosalpinx is an acutely inflamed blocked tube filled with pus. It sometimes subsides with antibiotics, becoming a hydrosalpinx. Otherwise it can rupture and form an abscess in the pelvis, much like a burst appendix, and then requires an operation to drain both it and the abscess.
ENDOMETRIOSIS
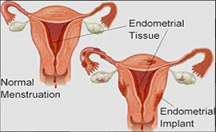
Endometriosis is a disorder of the female reproductive system, where endometrial tissue (the normal lining of the uterus) is found in areas other than the uterus. The most common sites are in the pelvis - the ovaries or tissues near the uterus and fallopian tubes, including the bladder, ligaments and bowel.
The exact causes of endometriosis are still not fully understood. It is believed that endometriosis occurs as a result of normal tissue from the uterus escaping into the fallopian tube and out into the pelvic area at the time of menstruation ("retrograde menstruation"). These tissue fragments are then thought to implant and grow onto the surrounding pelvic tissue and, sometimes, organs.
Because these fragments are made of the same tissue as the lining of the uterus, they too respond to the hormonal changes that occur during the menstrual cycle and, therefore, "bleed". Whereas menstrual blood can escape from the body, this has no exit and, as a result, the areas surrounding the implants of tissue become irritated or inflamed. Some of the blood and tissue may form into cysts (fluid filled lumps) - sometimes known as "chocolate" cysts, due to the colour similarity. The continual release of blood contributes to the formation of scar tissue. If the endometriosis is severe, bands of this scarred tissue ("adhesions") may develop.
Endometriosis and infertility are definitely related. And although some women with endometriosis remain fertile, endometriosis is regarded as one of the most common factors associating with infertility in women over 25 years. It has been further estimated that between a third and a half of all women with infertility problems have some degree of endometriosis.
Why it causes infertility is unclear. For women with severe endometriosis, their fallopian tubes may be so damaged that it is impossible for the egg to reach the sperm. Other women may have "chocolate cysts" on their ovaries which impair ovulation. But even where it is mild or where the endometriosis is not found on the tubes or ovaries, women can remain infertile.
Pain is the major symptom, though its intensity may vary. It may be experienced as a sharp stabbing pain, a constant or intermittent dull ache, or as a severe cramping pain.
This pain may be felt:
- with periods (mild, moderate or severe pain);
- during ovulation (mild, moderate or severe pain midway between periods).
- in the bowel during menstruation, or bowel movements or when passing wind;
- during or after sexual intercourse
Other symptoms may include:
- infertility;
- diarrhoea or constipation
- heavy or irregular bleeding (sometimes involving the loss of large clots of blood or tissue)
- pre-menstrual tension
The severity of your symptoms has little to do with the extent of your endometriosis. Some women may have severe pain from just a slight build-up of tissue, whereas other women may have only the mildest symptoms despite an extensive build-up of tissue.
The presence of endometriosis may be diagnosed at the initial consultation and examination, however, a firm diagnosis can be made when the endometriosis is actually seen, using a surgical procedure known as a laparoscopy. This enables the doctor to view the ovaries, fallopian tubes, uterus and other pelvic organs. Options for treatment may include no treatment at all (if the symptoms are tolerable), drug therapy or surgery.
- Drug Therapy
Drug therapy is used to supress ovulation and, therefore, menstuation. Some of the drugs used are the oral contraceptive pill, progesterones (which cause a pseudo-pregnancy), Duphaston (which causes a pseudo-menopause), Danazol, Synarel and Zoladex – a new once-monthly injectable drug. These drugs are not always effective.
These medications are usually taken for 6 months, depending on the severity of the condition. These synthetic hormones suppress the function of the ovaries by acting on the pituitary so that hormones necessary for ovulation are not produced. By keeping a woman free of menstruation ("pseudo-menopause") the endometrial tissue does not have a chance to bleed, thus enabling the inflamed areas to heal.
Possible side effects include weight gain of 1-4kgs, some decrease in breast size, a tendency towards acne, occasional increase in body hair, oily skin and symptoms of the menopause such as hot flushes and nausea. Symptoms should be reversible after the drug is discontinued. Normal ovulation and ovarian functions should return to normal following cessation of medication.
This treatment gives some women immediate and substantial relief from symptoms. Not every woman suffers from these side effects but for others the side effects can be worse than the original symptoms.
- Surgery
Where more severe forms of endometriosis exit, particularly where "chocolate cyst" formation in the ovary and tubal adhesions prevent normal egg transportation, surgery is indicated to restore normal anatomy as far as possible.
Surgical procedures may range from simple cautery of endometriosis spots to extensive removal of scar tissue and microsurgery. Surgical use of laser technology is also becoming more frequent.
A combination of surgical treatment and medication has been used with impressive results – up to 79% pregnancy rate in reported series
FIBROIDS AND LUMPS
Fibroids are benign lumps of tissue growing in or on the myometrium (the wall of the uterus surrounding the endometrium). The closer they are to the endometrium, the more likely they are to cause symptoms such as heavy bleeding, dysmenorrhea and infertility.
Enquire from us
Send an enquiry to us now and get a Free Consultation for your visit.